First-Pass Claim Acceptance: The Hidden Growth Engine for Healthcare Revenue
Introduction
For many healthcare organizations, revenue growth is often associated with increasing patient volume, expanding services, or negotiating better payer contracts. But one of the most powerful drivers of financial performance is often overlooked: first-pass claim acceptance rate.
Every claim that gets rejected, denied, or returned for correction adds administrative cost, delays cash flow, and increases operational burden. Improving first-pass acceptance is not just a billing improvement — it’s a revenue acceleration strategy.
In this article, we explore why first-pass claim acceptance matters, what impacts it, and how healthcare providers can dramatically improve performance.
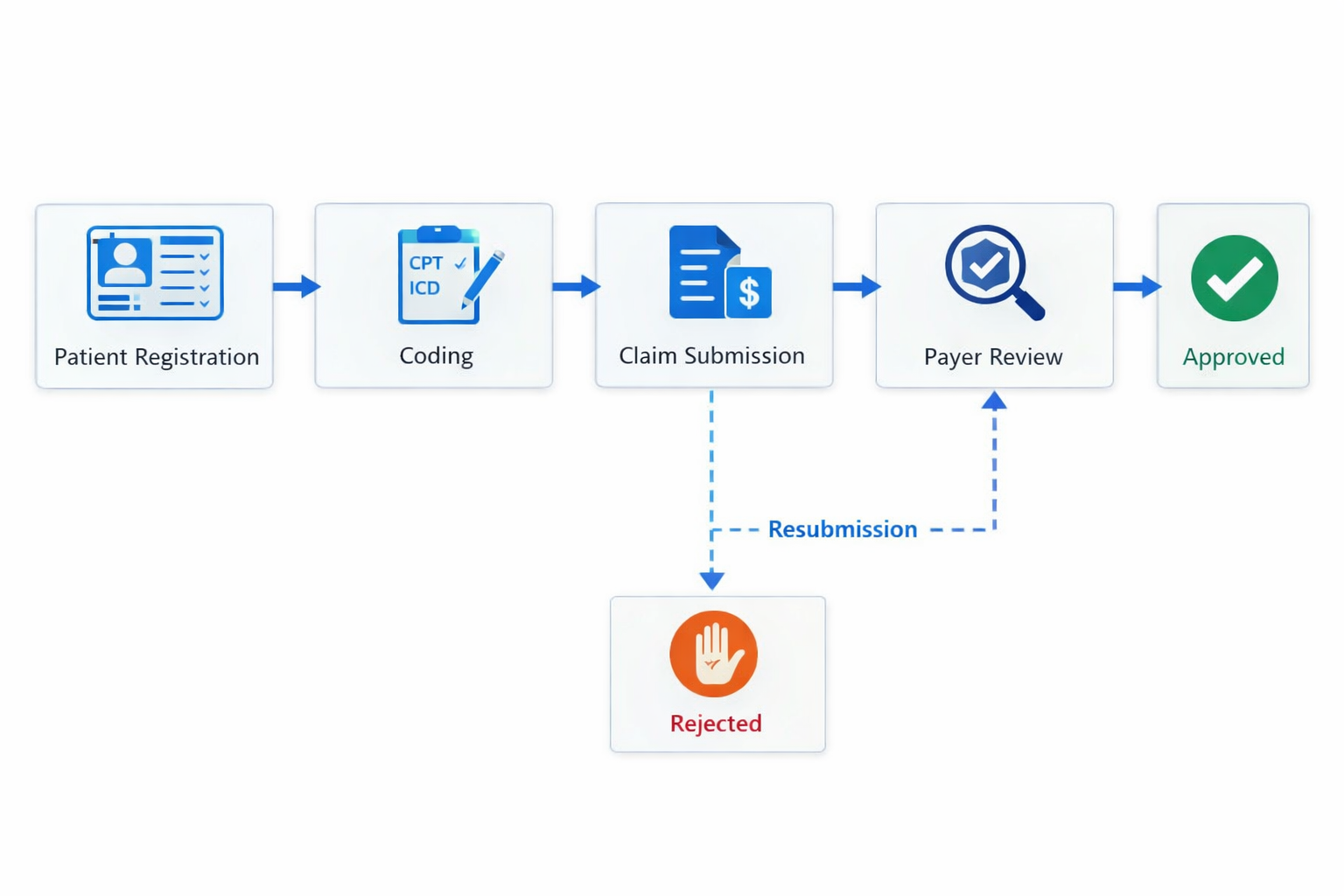
What Is First-Pass Claim Acceptance?
First-pass claim acceptance refers to the percentage of claims that are approved and processed by payers without requiring correction or resubmission.
A high rate means:
Faster reimbursements
Reduced administrative work
Lower denial management costs
Improved revenue predictability
A low rate creates friction at every stage of the revenue cycle.
Why First-Pass Acceptance Matters More Than Ever
1. Cash Flow Depends on Speed
Delayed claims mean delayed payments. Even small error rates can create major revenue bottlenecks when multiplied across thousands of claims.
2. Administrative Costs Add Up Quickly
Each rejected claim requires staff time for investigation, correction, and resubmission. This increases labor costs and reduces operational efficiency.
3. Denials Are Getting More Complex
Payer requirements continue to evolve. Without strong validation and compliance processes, error rates naturally increase.
4. Revenue Leakage Is Often Invisible
Many organizations focus on denial recovery but overlook prevention. Preventing rejections before submission is significantly more cost-effective.
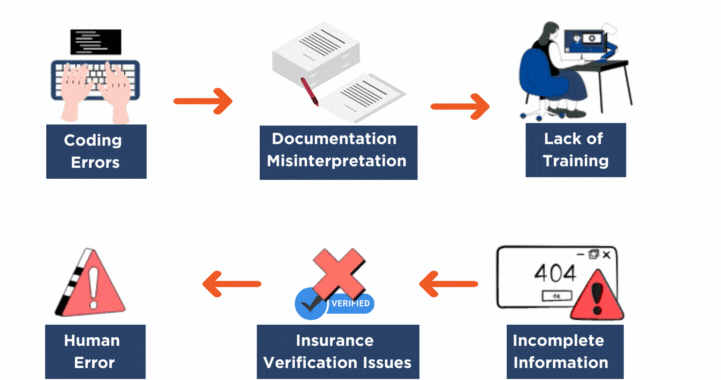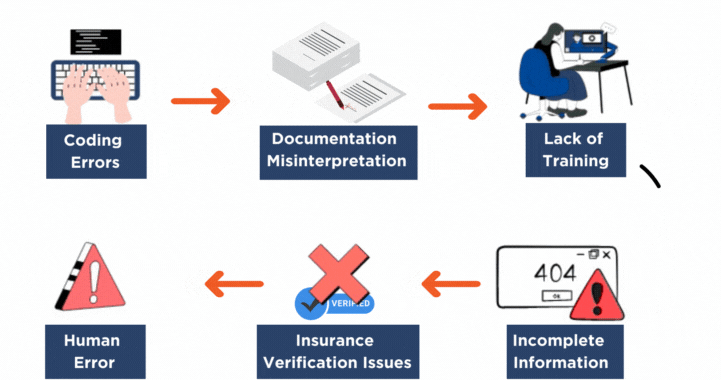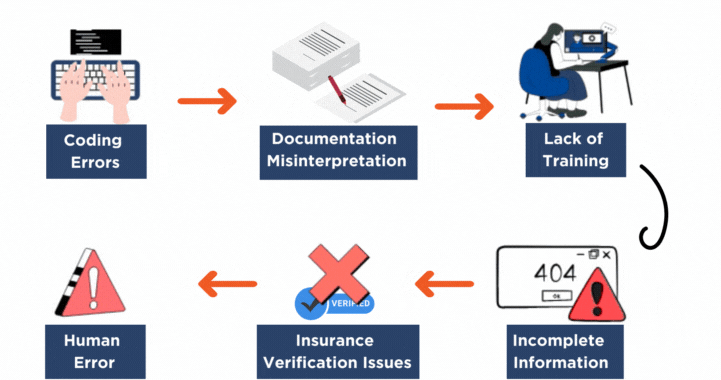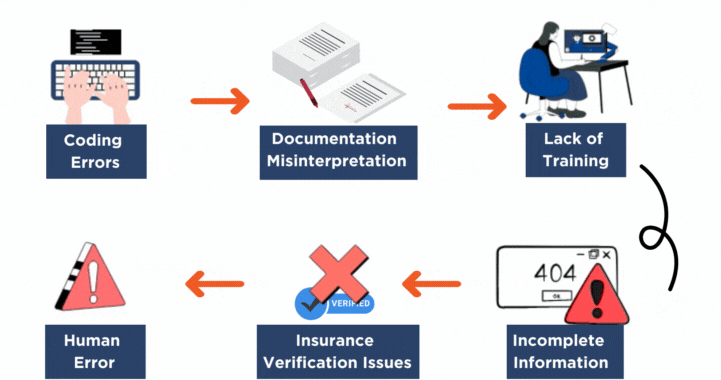
The Most Common Causes of Claim Rejections
Healthcare providers typically see rejections due to:
Incomplete patient information
Eligibility verification errors
Incorrect coding or missing modifiers
Documentation gaps
Authorization issues
Payer-specific rule violations
Most of these are preventable before submission.
How to Improve First-Pass Claim Acceptance
1. Strengthen Front-End Data Accuracy
Accurate patient registration and eligibility verification are foundational. Errors at intake ripple through the entire revenue cycle.
2. Implement Real-Time Claim Validation
Automated claim scrubbing identifies errors before submission, reducing preventable rejections.
3. Standardize Coding Quality Control
Regular coding audits and documentation reviews ensure compliance and accuracy.
4. Monitor Payer Trends Continuously
Tracking denial patterns reveals root causes and enables targeted process improvements.
5. Align People, Process, and Technology
Technology alone is not enough. High performance requires skilled teams, structured workflows, and continuous monitoring.
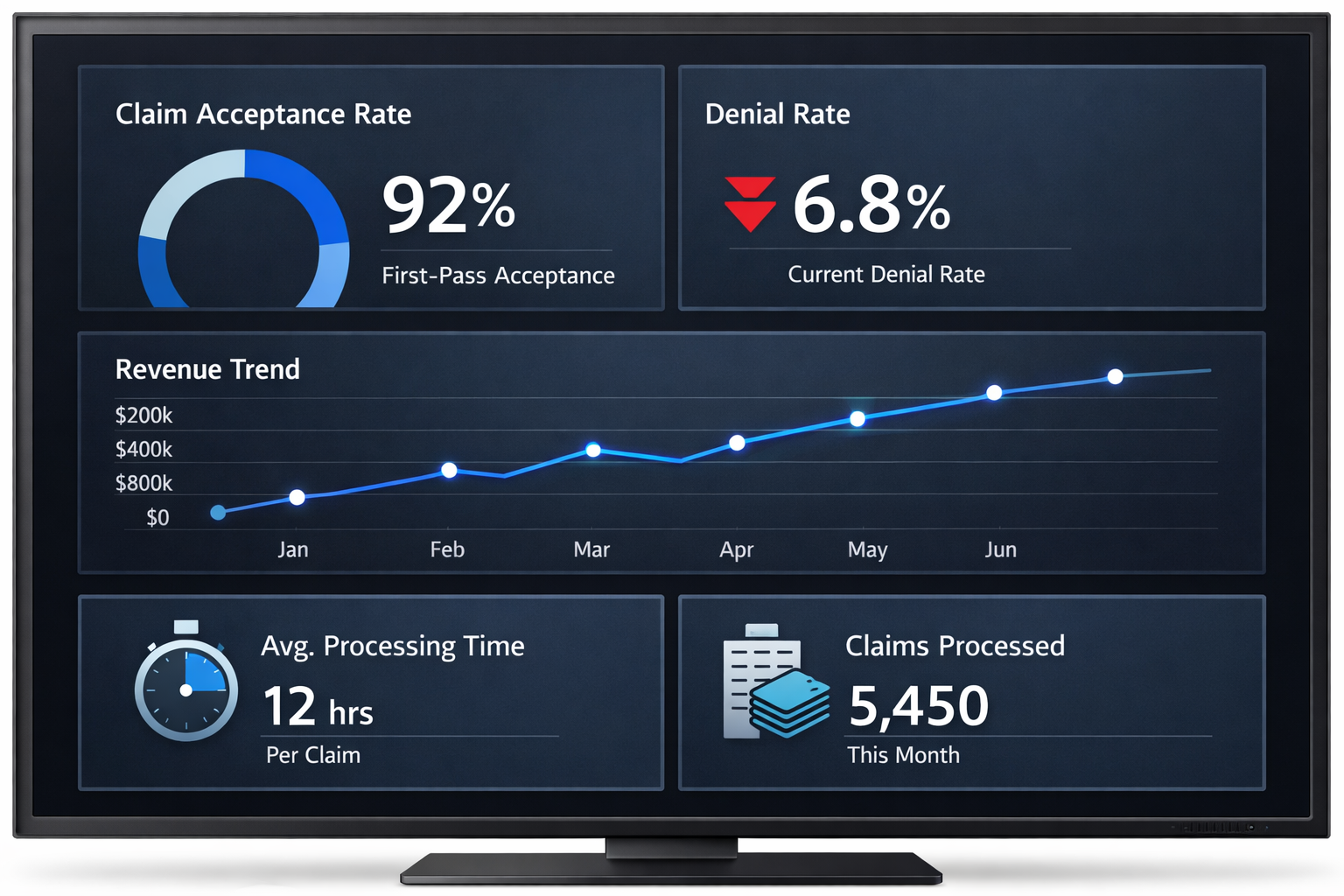
The Financial Impact of Higher First-Pass Rates
Healthcare organizations that optimize claim acceptance typically experience:
Faster reimbursement cycles
Lower cost per claim processed
Reduced denial rates
Improved staff productivity
More predictable revenue forecasting
Even a small percentage improvement can produce significant annual financial gains.
Prevention Is the New Revenue Strategy
Traditionally, denial management focused on fixing problems after they occurred. Today, leading healthcare organizations prioritize denial prevention and clean claim submission.
The shift is simple:
Fixing errors costs money.
Preventing errors creates revenue velocity.
Final Thoughts
First-pass claim acceptance is more than a billing metric — it’s a strategic performance indicator that reflects operational discipline, data accuracy, and revenue cycle maturity.
Healthcare providers that prioritize clean claim submission don’t just reduce denials. They unlock faster cash flow, lower costs, and scalable financial growth.
In today’s complex reimbursement environment, improving first-pass acceptance is one of the most effective ways to strengthen long-term financial performance.